Understanding Your Menstrual Cycle
The menstrual cycle is a natural process that occurs in the female reproductive system. It involves a series of hormonal and physical changes that prepare the body for potential pregnancy. Understanding your menstrual cycle can empower you to take control of your reproductive health and make informed decisions about contraception, family planning, and overall well-being.
What is the Menstrual Cycle?
The menstrual cycle refers to the monthly changes that happen in a woman’s body in preparation for pregnancy. Each cycle typically lasts between 21 and 35 days and is counted from the first day of one period to the first day of the next. The cycle can be divided into four phases:
1. Menstruation (Day 1-5)
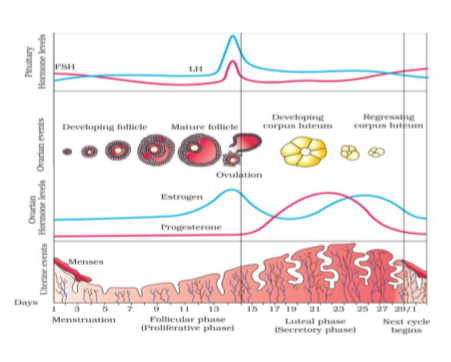
This phase marks the start of the menstrual cycle. During menstruation, the lining of the uterus sheds and is expelled from the body. This results in bleeding, which can last anywhere from 3 to 7 days.
2. Follicular Phase (Day 1-14)
The follicular phase begins on the first day of menstruation and lasts until ovulation. During this phase, several follicles in the ovaries start to develop and mature. These follicles release estrogen, which stimulates the thickening of the uterine lining in preparation for pregnancy.
3. Ovulation (Day 14)
Ovulation is the release of a mature egg from the ovary. This usually occurs around day 14 of a 28-day cycle. The egg travels down the fallopian tube, where it can be fertilized by sperm if sexual intercourse takes place.
4. Luteal Phase (Day 15-28)
The luteal phase begins after ovulation and lasts until the start of the next menstrual cycle. During this phase, the ruptured follicle transforms into a structure called the corpus luteum, which releases progesterone. Progesterone helps prepare the uterus for potential implantation of a fertilized egg. If pregnancy does not occur, hormone levels drop, and the cycle starts again with menstruation.
What Affects Your Menstrual Cycle?
Several factors can influence the regularity and characteristics of your menstrual cycle, including:
Hormonal Imbalances
Hormonal imbalances, such as polycystic ovary syndrome (PCOS) or thyroid disorders, can disrupt the normal functioning of the menstrual cycle. These imbalances can cause irregular periods, heavy or light bleeding, or even a lack of menstruation.
Stress
Emotional and physical stress can impact hormone production and disrupt the menstrual cycle. High-stress levels may cause missed periods, delayed ovulation, or irregular bleeding.
Diet and Exercise
Poor nutrition or excessive exercise can significantly affect your menstrual cycle. Extreme weight loss or gain can lead to irregular periods or even stop menstruation altogether.
Tracking Your Menstrual Cycle
Keeping track of your menstrual cycle can provide valuable insights into your reproductive health. There are various methods to track your cycle:
Calendar Tracking
Using a calendar or a period-tracking app, you can record the start and end dates of your periods. Over time, this can help you identify patterns and irregularities in your menstrual cycle.
Basal Body Temperature (BBT) Charting
BBT charting involves taking your body temperature every morning before getting out of bed. Your basal body temperature rises slightly after ovulation, indicating the most fertile phase of your cycle.
Cervical Mucus Monitoring
Throughout your cycle, the consistency and appearance of your cervical mucus change. By monitoring these changes, you can identify the times when you are most likely to be fertile.
Conclusion
Understanding your menstrual cycle is essential for maintaining your overall reproductive health. By tracking your cycle and paying attention to any changes or irregularities, you can better understand your body, detect potential issues, and make informed decisions about your reproductive well-being.